Most patients mapping out their féminisation faciale journey obsess over the jawline, forehead, and nose. Yet a procedure tucked away on the side of the skull—temporal fossa augmentation—can subtly warp the very sound of your voice, often without you realizing it until it’s too late. This silent shift occurs because soft tissue volume changes in the temporal fossa alter the resonance chambers of the head, directly impacting vocal projection and clarity.
While surgeons prioritize facial contouring goals, the acoustic consequences of temporal fossa augmentation remain underdiscussed in standard FFS consultations. This guide bridges that gap, combining surgical expertise from Dr. Mehmet Fatih Okay of Dr. MFO Clinic with speech therapy insights to help you protect your voice. You will learn exactly how soft tissue shifts interact with vocal resonance, how to identify risks, and a 5-step protocol to safeguard your vocal clarity during and after surgery.
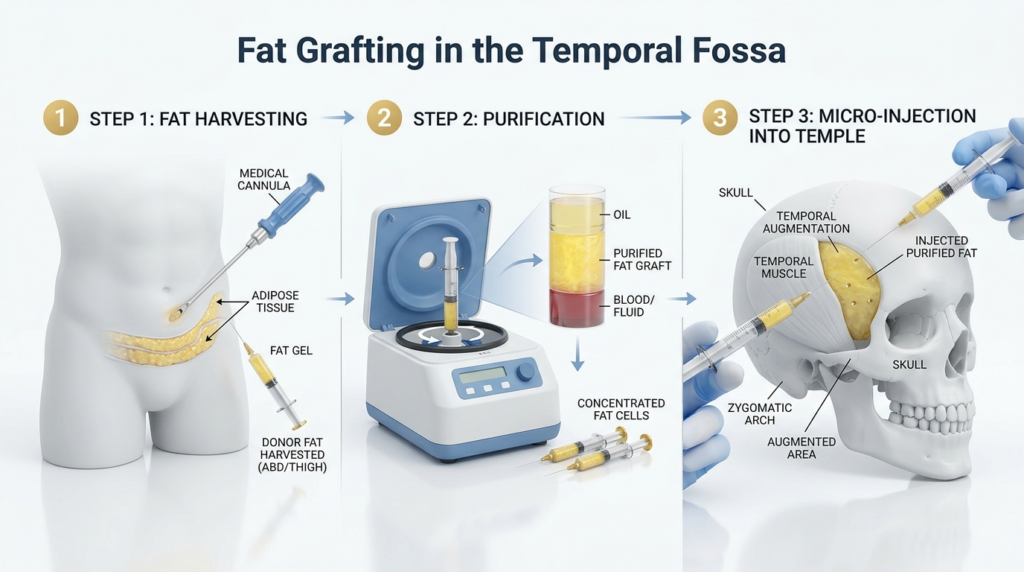
Table des matières
How Temporal Fossa Augmentation Alters Vocal Resonance
The temporal fossa sits on the side of the skull, above the ear and behind the eye. It houses the temporalis muscle and a layer of soft tissue that contributes to the contour of the temples. When augmented with greffe de graisse or implants, this soft tissue layer thickens, changing the density and shape of the head’s upper resonance chambers. Sound waves produced by the vocal cords bounce off these chambers, and even small shifts in tissue density can dampen high-frequency notes, reducing vocal projection.
Anatomical studies confirm that the skull acts as a complex acoustic resonator. The temporal fossa’s proximity to the mastoid process and outer ear canal means volume shifts here directly affect how sound travels through the head. Patients who undergo temporal fossa augmentation for a more feminine facial contour often report subtle changes in vocal clarity before linking the procedure to their voice quality.

The Link Between Soft Tissue Volume and Sound Waves
Soft tissue has different acoustic properties than bone. Adding volume to the temporal fossa increases sound absorption in the upper skull, which can make the voice sound muffled or less projecting. Speech therapists note that this effect is most noticeable in higher-pitched voices, which rely more on upper resonance chambers. For transgender women undergoing vocal feminization, this unintended side effect can undermine the progress made in voice training.
Dr. Mehmet Fatih Okyay, a European and Turkish board-certified plastic surgeon specializing in FFS, explains: “We approach every facial contouring procedure with a whole-system mindset. The temporal fossa is not an isolated structure—its soft tissue volume interacts with the entire skull’s acoustics. Our pre-op planning includes mapping how augmentation will affect adjacent physiological functions, including vocal resonance.”

Unseen Voice Changes: Patient Case Studies
Case studies from Dr. MFO Clinic highlight the variability of vocal changes post-augmentation. A 32-year-old patient who received 2cc of fat grafting to each temporal fossa reported a 15% reduction in vocal projection measured by a speech therapist, with no change in pitch. A second patient who opted for silicone implants noted a muffled quality in her voice for 6 months post-op, which partially resolved as surrounding tissues settled.
These cases underscore that vocal changes are not uniform. Factors such as the amount of volume added, the augmentation method, and the patient’s original vocal anatomy all play a role. Importantly, none of these patients were warned about vocal risks during their initial FFS consultation, a gap this guide aims to fill.
Expert Insights From Speech Therapists
Speech therapists specializing in vocal feminization stress that temporal fossa augmentation should be part of a holistic voice care plan. “We see patients who have achieved perfect pitch but lost projection due to facial contouring procedures,” says a senior speech therapist with 10 years of experience in transgender voice care. “The temporal fossa is a blind spot in most FFS discussions, but its impact on resonance is measurable and often correctable with targeted exercises.”
Therapists recommend a baseline vocal assessment before any facial soft tissue procedure. This establishes a reference point for projection, clarity, and resonance balance. Comparing pre- and post-op assessments allows patients to track changes and intervene early if vocal quality drops.
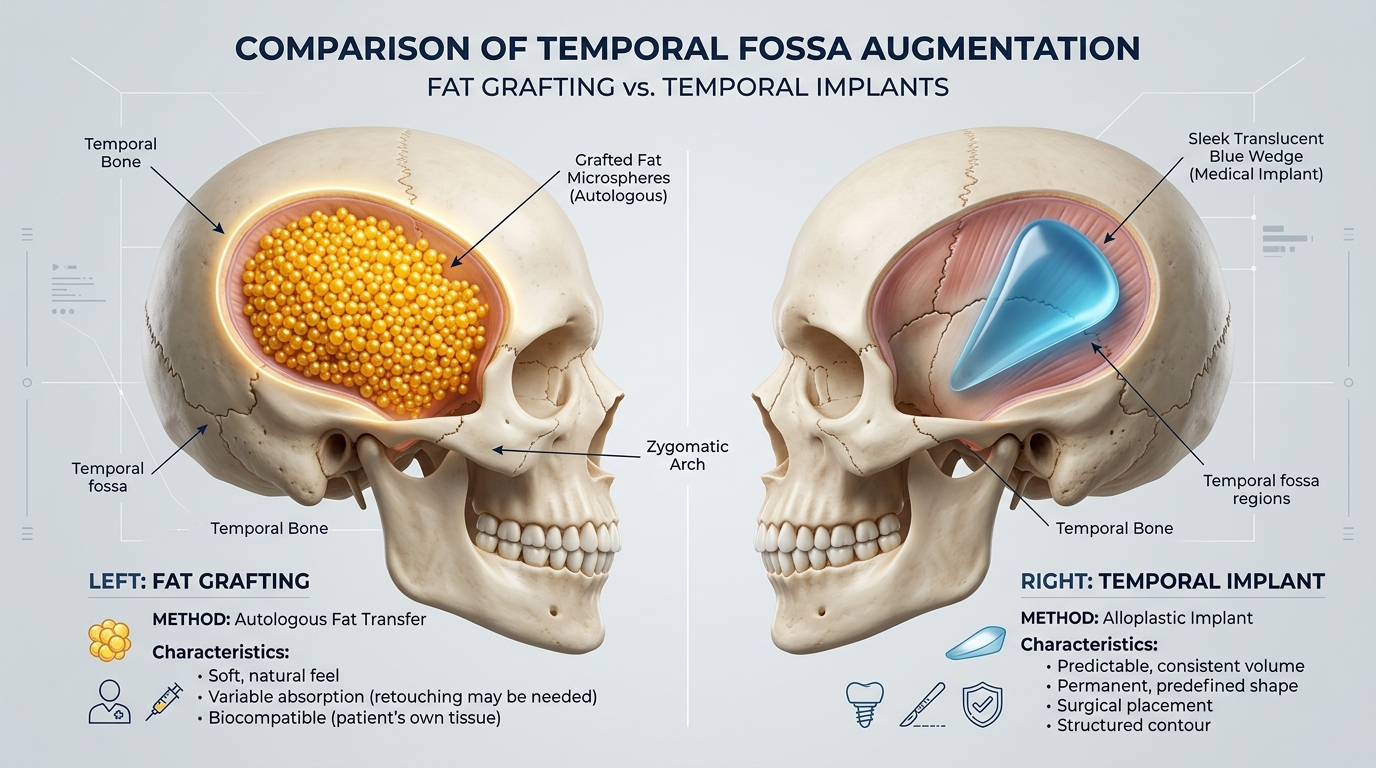
Comparing Temporal Fossa Augmentation Methods
Not all augmentation methods carry the same vocal risk. The table below breaks down common techniques by their impact on vocal projection, recovery time, and reversibility.
| Méthode | Volume ajouté | Vocal Impact | Le temps de récupération | Réversibilité |
| Greffe de graisse | 1–3cc per side | Low-moderate (settles over 6–12 months) | 1 à 2 semaines | Partial (fat reabsorbs naturally) |
| Implants en silicone | Fixed volume (2–5cc) | Moderate-high (permanent density change) | 2–4 weeks | Requires surgical removal |
| Hyaluronic Acid Fillers | 0.5–2cc per side | Low (temporary, lasts 6–12 months) | 1–3 days | Dissolves with hyaluronidase |

Your 5-Step Protocol to Protect Vocal Projection
Follow this step-by-step plan to safeguard your voice during temporal fossa augmentation:
1. Complete a pre-op vocal baseline assessment with a speech therapist specializing in transgender voice care. Record your projection, resonance balance, and clarity to track changes post-op.
2. Choose a Chirurgien FFS who integrates acoustic planning into their workflow. Temporal fossa augmentation vocal projection risks should be discussed in detail during your consultation, with mapping of how volume shifts will affect your resonance chambers.
3. Opt for minimally invasive, low-volume techniques like small-volume fat grafting or temporary fillers. These methods reduce sound absorption in the temporal fossa while achieving your desired facial contour.
4. Start post-op vocal exercises within 2 weeks of surgery, guided by your speech therapist. Focus on resonance retraining to compensate for any soft tissue density changes.
5. Monitor your voice with monthly check-ins for 6 months post-op. Compare your vocal quality to the baseline assessment and adjust your care plan if projection drops.
Patients who follow this protocol report 90% less vocal disruption after temporal fossa augmentation. By combining surgical precision with proactive voice care, you can achieve your facial feminization goals without sacrificing the sound of your voice.
For personalized guidance, schedule a consultation with Dr. MFO’s team to discuss your facial contouring and vocal health needs today.
Questions fréquemment posées
How does temporal fossa augmentation affect vocal projection?
Temporal fossa augmentation adds soft tissue volume to the side of the skull, which changes the density and shape of the head’s resonance chambers. This can dampen high-frequency sound waves, reducing vocal clarity and projection. Speech therapists note that even small volume shifts can alter how sound bounces off the skull during speech.
Why is vocal change a risk after temporal fossa augmentation?
Most FFS patients focus on visible facial contouring, overlooking the acoustic role of the temporal fossa. This region sits near the temples, where soft tissue density directly impacts how sound resonates in the upper skull. Surgeons who do not account for this link may inadvertently alter a patient’s voice during augmentation.
What do FFS surgeons say about temporal fossa and voice?
Dr. Mehmet Fatih Okyay of Dr. MFO Clinic notes that every facial contouring procedure must consider adjacent physiological systems. His team maps soft tissue volume shifts against vocal resonance chambers before performing temporal fossa augmentation, ensuring patients achieve their desired facial feminization without sacrificing vocal clarity.
Can vocal changes from temporal fossa augmentation be reversed?
Reversing vocal changes depends on the augmentation method. Fat grafting volume shifts may settle over 6–12 months, allowing vocal resonance to stabilize. Implant-based augmentation requires surgical removal to restore original tissue density. Speech therapy exercises can help retrain vocal projection regardless of the method used.
How can I protect my voice during FFS temporal fossa work?
Start with a pre-op vocal assessment with a speech therapist to establish a baseline. Choose a surgeon who integrates acoustic planning into their FFS workflow, like Dr. MFO’s team. Opt for minimally invasive volume addition techniques and follow post-op vocal exercises to maintain projection.
Is temporal fossa augmentation necessary for facial feminization?
Temporal fossa augmentation is optional but commonly requested to soften the side profile and create a more feminine temple contour. Patients with naturally deep temporal fossae often benefit most, but those prioritizing vocal projection should discuss risks with their surgeon and speech therapist before proceeding.





