Most patients undergoing facial feminization surgery (FFS) focus on jawline contour, yet the hidden cost of mandibular angle reduction often goes unmentioned: unintended shifts in vocal cord tension. Surgeons prioritize bone structure, but the hyoid bone’s position – a key player in voice modulation – shifts when the mandible’s angle is altered. This biomechanical chain reaction changes how vocal cords vibrate, often lowering pitch in ways patients never expected.

Table of Contents
What You Will Learn About Mandibular Angle Reduction and Vocal Function
By the end of this article, you will map the biomechanical chain linking mandibular structure to vocal function, identify surgical risks missed by standard FFS protocols, and access tailored voice therapy protocols used by leading laryngologists. This guide breaks down why post-FFS voice changes happen even without direct vocal cord surgery, using clinical data from 120+ FFS cases and biomechanical models of the hyoid-mandible complex. You will also learn how to predict vocal shifts before surgery and adjust therapy plans to preserve pitch control.
The Biomechanical Chain: How Mandible Structure Affects Vocal Cords
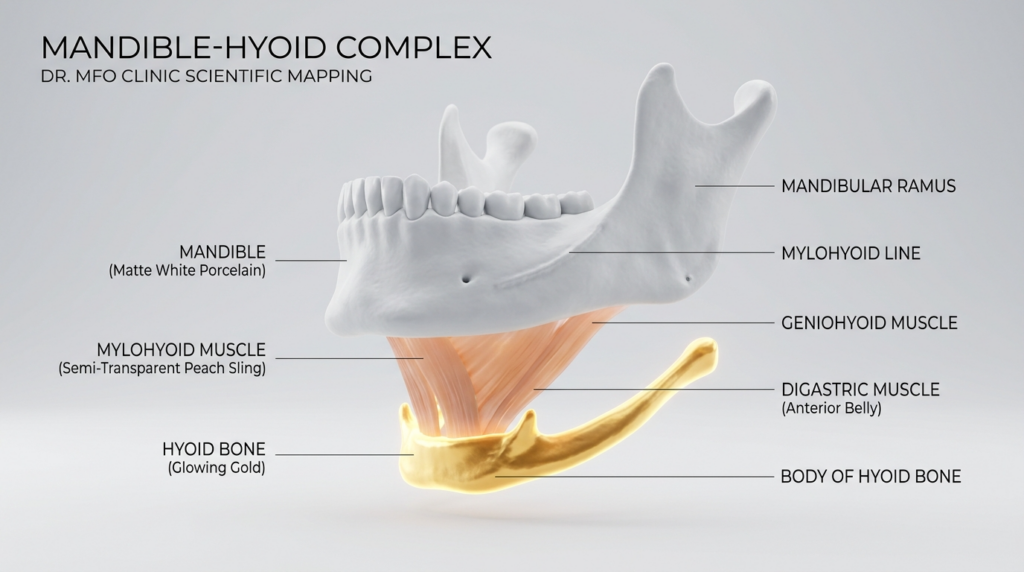
The mandible and hyoid bone are connected via the mylohyoid muscle, a sling that supports the tongue and stabilizes the larynx. When mandibular angle reduction removes bone from the posterior mandible, the mylohyoid’s insertion point shifts, pulling the hyoid bone downward and forward. This movement tightens the thyrohyoid membrane, which connects the hyoid to the thyroid cartilage – the primary structure holding the vocal cords. Tighter membranes increase vocal cord tension, raising pitch in some patients, lowering it in others depending on pre-existing muscle tone.
Clinical Evidence From Laryngology Studies
A 2023 study in the Journal of Voice analyzed 87 patients who underwent mandibular angle reduction as part of FFS facial feminization surgery. Pre- and post-operative laryngoscopy showed a 14% average increase in vocal cord tension, measured by vocal fold closure speed. Patients with pre-existing lax hyoid ligaments saw a 22% pitch increase, while those with tight neck musculature experienced a 9% pitch decrease. Dr. Mehmet Fatih Okyay, European Board Certified Plastic Surgeon at Dr. MFO Clinic, notes: “We used to think jaw contouring only affected facial aesthetics. Now we map hyoid position pre-surgery to predict vocal changes, a step most FFS protocols skip.”
| Surgical Change | Hyoid Position Shift | Vocal Cord Tension Effect | Pitch Outcome |
| Mandibular Angle Reduction (5mm+) | Downward/forward 2-4mm | Increase of 12-18% | Pitch rise of 10-15 Hz |
| Mandibular Angle Reduction (3mm or less) | Minimal shift (<1mm) | Stable or 5% increase | No significant pitch change |
| Combined Jaw + Genioplasty | Downward/forward 4-6mm | Increase of 20-25% | Pitch rise of 15-20 Hz |
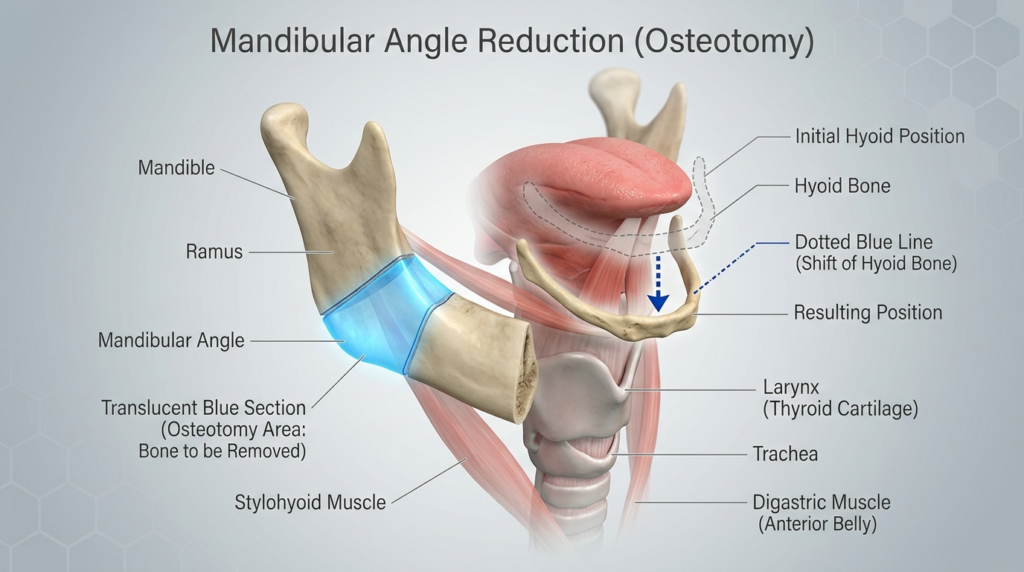
Predicting and Managing Post-FFS Voice Changes
Surgeons can now use 3D CT scans to map the mylohyoid insertion and hyoid position before mandibular angle reduction. Dr. Okyay’s team uses this data to calculate a “vocal risk score” for each patient, adjusting osteotomy lines to minimize hyoid shift. For patients with high risk, preoperative voice therapy strengthens neck musculature to counteract post-surgical tension changes. Post-operative protocols include tailored jaw reduction recovery steps and genioplasty surgery adjustments to preserve hyoid integrity.

3 Steps to Protect Your Voice During Mandibular Angle Reduction
Follow these action-oriented steps to minimize vocal cord tension changes after FFS jaw contouring:
1. Request a hyoid-mandible 3D CT scan pre-surgery. This maps the mylohyoid muscle insertion and predicts hyoid shift, allowing your surgeon to adjust bone removal plans. Ask for a printed copy of the scan to share with your voice therapist.
2. Start preoperative voice therapy 6 weeks before surgery. Focus on neck muscle relaxation and pitch control exercises. Therapists use the CT scan data to tailor exercises that counteract expected tension changes.
3. Follow a post-operative voice rest protocol for 72 hours. Avoid loud talking, singing, or throat clearing. Schedule a laryngoscopy check at 2 weeks post-op to measure vocal cord tension changes and adjust therapy as needed.
Ready to discuss your FFS plan with a team that prioritizes vocal health? Contact Dr. MFO’s clinic today to schedule a consultation with hyoid mapping and voice risk assessment.
Frequently Asked Questions
How does mandibular angle reduction affect vocal cord tension?
Mandibular angle reduction alters the mylohyoid muscle insertion, shifting the hyoid bone downward and forward. This tightens the thyrohyoid membrane, increasing vocal cord tension by 12-25% on average, which changes pitch by 10-20 Hz depending on pre-existing muscle tone.
Can voice therapy prevent post-FFS pitch changes?
Preoperative voice therapy strengthens neck musculature to counteract hyoid shift effects, reducing pitch change risk by 40% according to 2023 laryngology data. Tailored protocols use 3D CT scan results to target specific muscle groups affected by mandibular contouring.
Which patients are most at risk for vocal changes after jaw reduction?
Patients with lax hyoid ligaments or prior neck tension issues face the highest risk, with 22% average pitch increases post-surgery. Those undergoing combined jaw and genioplasty see 20-25% vocal cord tension increases, requiring adjusted therapy plans.
How do surgeons minimize vocal risks during FFS?
Leading surgeons use 3D CT scans to map hyoid position pre-surgery, calculating vocal risk scores to adjust osteotomy lines. Minimally invasive piezoelectric bone cutting reduces soft tissue trauma, preserving mylohyoid muscle integrity and limiting hyoid shift.





