Chondrolaryngoplasty, commonly referred to as a tracheal shave, is a pivotal procedure in gender-affirming care for transgender women. By reducing the prominence of the Adam’s apple (thyroid cartilage), this surgery aligns facial features with feminine aesthetics, enhancing both physical appearance and psychological well-being. However, as with any surgical intervention, safety, efficacy, and long-term outcomes remain paramount. This guide explores the latest advancements, risks, and best practices in chondrolaryngoplasty, ensuring patients and practitioners alike are equipped with the knowledge needed for informed decision-making.
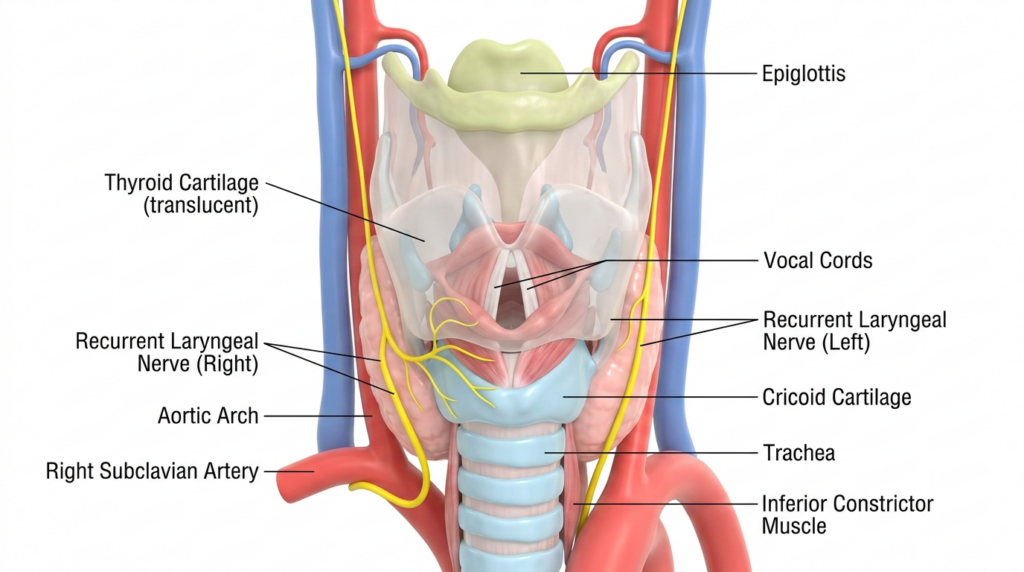
Table of Contents
The Anatomy of the Adam’s Apple and Surgical Objectives
The Adam’s apple, or thyroid cartilage, is a prominent feature of the male neck, resulting from testosterone-induced growth during puberty. For transgender women, its reduction is often a critical step in achieving a more feminine neck contour. The primary goal of chondrolaryngoplasty is to reduce the anterior projection of the thyroid cartilage while preserving vocal cord function and minimizing scarring. This requires a deep understanding of laryngeal anatomy and meticulous surgical precision.
Key anatomical considerations include:
- Thyroid Cartilage: The largest cartilage of the larynx, forming the Adam’s apple. Its reduction must avoid damage to the vocal cords.
- Cricoid Cartilage: Located below the thyroid cartilage, it plays a role in airway protection and must remain intact.
- Recurrent Laryngeal Nerve: A critical nerve that controls vocal cord movement. Injury to this nerve can result in voice changes or breathing difficulties.
Surgical Techniques: Balancing Aesthetics and Safety
Modern chondrolaryngoplasty employs advanced techniques to ensure both aesthetic success and patient safety. The procedure typically involves:
1. Preoperative Planning: High-resolution imaging, such as CT scans, maps the thyroid cartilage’s structure and its relationship with surrounding tissues. This step is crucial for identifying potential risks and tailoring the surgical approach.
2. Surgical Approach: A small horizontal incision is made in a natural skin crease to minimize visible scarring. The thyroid cartilage is then carefully reshaped using specialized instruments, such as piezoelectric devices, which reduce the risk of thermal damage to surrounding tissues.
3. Vocal Cord Protection: The procedure avoids deep incisions near the vocal cords. Surgeons use intraoperative nerve monitoring to ensure the recurrent laryngeal nerve remains unharmed, preserving voice quality.
4. Closure and Recovery: The incision is closed with dissolvable sutures, and patients are provided with detailed post-operative care instructions to promote healing and minimize complications.
Risks and Complications: What Patients Need to Know
While chondrolaryngoplasty is generally safe, it is not without risks. Understanding these potential complications is essential for patients considering the procedure:
1. Voice Changes: Temporary hoarseness or pitch alterations may occur due to swelling or minor nerve irritation. These changes typically resolve within weeks.
2. Nerve Injury: Although rare, damage to the recurrent laryngeal nerve can lead to permanent voice changes or breathing difficulties. Choosing an experienced surgeon significantly reduces this risk.
3. Scarring: While incisions are placed in natural skin folds, individual healing responses vary. Proper wound care and silicone gel application can minimize scar visibility.
4. Infection and Hematoma: As with any surgery, there is a risk of infection or bleeding. Adhering to post-operative care instructions and attending follow-up appointments mitigates these risks.

Post-Operative Care: Ensuring Optimal Recovery
Recovery from chondrolaryngoplasty is typically smooth, but adherence to post-operative guidelines is critical for optimal outcomes. Patients should:
- Avoid Straining the Neck: Refrain from heavy lifting or vigorous activities for at least two weeks to prevent tension on the incision.
- Follow a Soft Diet: Consume cool, soft foods to minimize discomfort and reduce swelling.
- Monitor for Complications: Report any signs of infection, excessive swelling, or voice changes to the surgical team immediately.
- Attend Follow-Up Appointments: Regular check-ups allow the surgeon to assess healing progress and address any concerns.
Most patients resume normal activities within 7–10 days, with full recovery achieved in 4–6 weeks.
Choosing the Right Surgeon: Why Experience Matters
Selecting a surgeon with specialized experience in gender-affirming procedures is the most critical factor in achieving safe and satisfactory outcomes. An expert surgeon will:
- Utilize Advanced Imaging: Employ 3D CT scans to map the thyroid cartilage and surrounding structures, ensuring precise surgical planning.
- Prioritize Nerve Protection: Use intraoperative nerve monitoring and piezoelectric instruments to safeguard the recurrent laryngeal nerve.
- Provide Transparent Communication: Discuss potential risks, expected outcomes, and recovery protocols in detail during the consultation.
- Offer Comprehensive Aftercare: Provide personalized post-operative care plans and remain accessible for follow-up questions or concerns.
Patients are encouraged to review before-and-after galleries, such as those found on Dr. MFO’s FFS Gallery, and seek consultations to ensure their surgeon’s expertise aligns with their goals.
Frequently Asked Questions
What is the primary goal of chondrolaryngoplasty?
The primary goal of chondrolaryngoplasty is to reduce the prominence of the Adam’s apple (thyroid cartilage) to create a more feminine neck contour while preserving vocal cord function and minimizing scarring.
How long does recovery take after chondrolaryngoplasty?
Most patients resume normal activities within 7–10 days, with full recovery typically achieved in 4–6 weeks. Adherence to post-operative care instructions is essential for optimal healing.
Are there risks of permanent voice changes after the procedure?
While temporary voice changes are common, permanent alterations are rare. Choosing an experienced surgeon who prioritizes nerve protection significantly reduces this risk.
What can I do to minimize scarring after surgery?
Proper wound care, including the use of silicone gel and avoiding sun exposure, can minimize scar visibility. Following your surgeon’s post-operative instructions is crucial.
Why is it important to choose a surgeon with experience in gender-affirming care?
A surgeon with specialized experience in gender-affirming procedures understands the unique anatomical and psychological considerations involved. This expertise ensures safer, more effective outcomes tailored to the patient’s goals.





